Building a fairer future: Advancing health equity through impact investment


Conference Programme
Healthy City Design 2024 (HCD 2024) International Congress & Exhibition is a global forum for the exchange of knowledge on the research, policy and practice of designing healthy and sustainable cities and communities.
Now in its 8th year and hosted for the second year running in the historical maritime port of Liverpool, this year’s Congress plenary theme is, ‘Building a fairer future: Advancing health equity through impact investment’.
The congress attracts researchers, practitioners, community voices, investors and policy makers from around the world committed to advancing health equity and sustainable development at the centre of the way we plan, develop and invest in our cities and urban communities.
We invite you to download this year's Call for Papers and submit abstracts on the core themes by 23 May using the online form.
Programme Committee


Prof Jeremy Myerson


Rachel Cooper PhD


Michael Parsons


Giselle Sebag, MPH, LEED AP, Fitwel Ambassador


Carolyn Daher MPH


Rhiannon Corcoran PhD


Marcus Grant


Harry Knibb


Rebecca Morley


Caroline Paradise PhD


Angela Loder


Audrey de Nazelle PhD


Mark Drane


Jose Siri PhD, MPH


Helen Pineo


Magali Thomson


Clare Wildfire


Jeri Brittin PhD


Blake Jackson AIA, LEED Fellow, WELL Faculty, CPHC

Awards Programme
In the past few years, we have presented 'best in class' awards in the closing session of the Healthy City Design Congress, in categories including 'Best Research Paper', 'Best Poster', and 'Most Innovative Idea'.
This year, we will be launching a new awards programme, celebrating and recognising the most innovative and impactful development projects across the urban design and planning, housing, transport and workplace sectors, as well as a dedicated design research award.
Keep an eye out in our newsletter and on this website, as we launch the Call for Entries for the Healthy City Design Awards at the end of April, or contact info@salus.global to learn more.



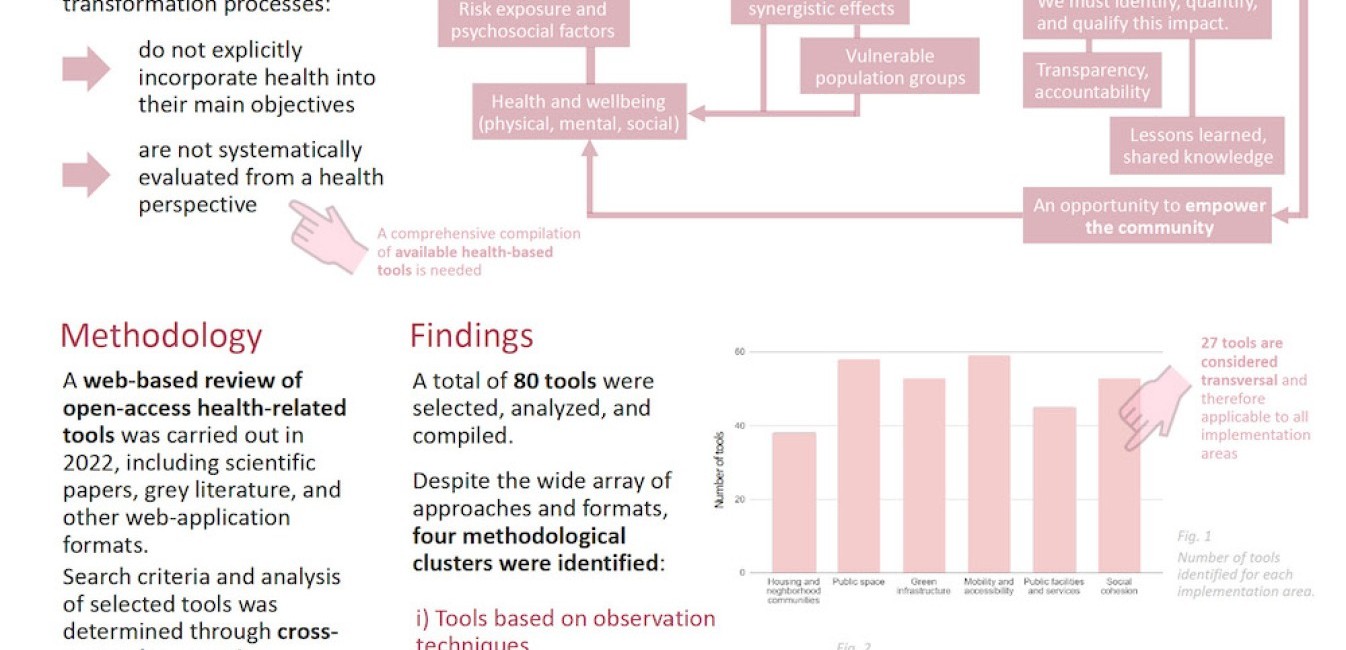
The ‘Best Research Paper’ category – for the paper that addresses the Congress theme of ‘Urban renewal and health equity’ in the most original and thorough way – was awarded to Ruth Gow and Celia Garcia of Bax & Company, from Spain. The authors’ paper demonstrated the Healthy Cities Generator tool, which helps practitioners, local authorities, citizens, and researchers understand the…